Wait times for medical procedures across Canada are some of the longest in the developed world and are far longer than they used to be. A shortage of doctors is often cited as a primary factor behind this problem.
It’s certainly true that hiring more doctors would help, but that may not be the best, or most cost-effective, solution to long and growing wait times. There are significant opportunities for Canada (or, more accurately, provincial governments) to better equip and support the doctors it already has by focusing on operational efficiencies, centralizing the waiting list system, and lessening the administrative burden doctors face.
In this commentary, we’ll look at how the number of physicians in Alberta and across Canada has changed over time to explore how a shortage of doctors alone does not explain worsening wait times. We’ll then discuss how wait times can be shortened in ways that make the most of the doctors Canada already has.
How has the number of doctors changed over time?
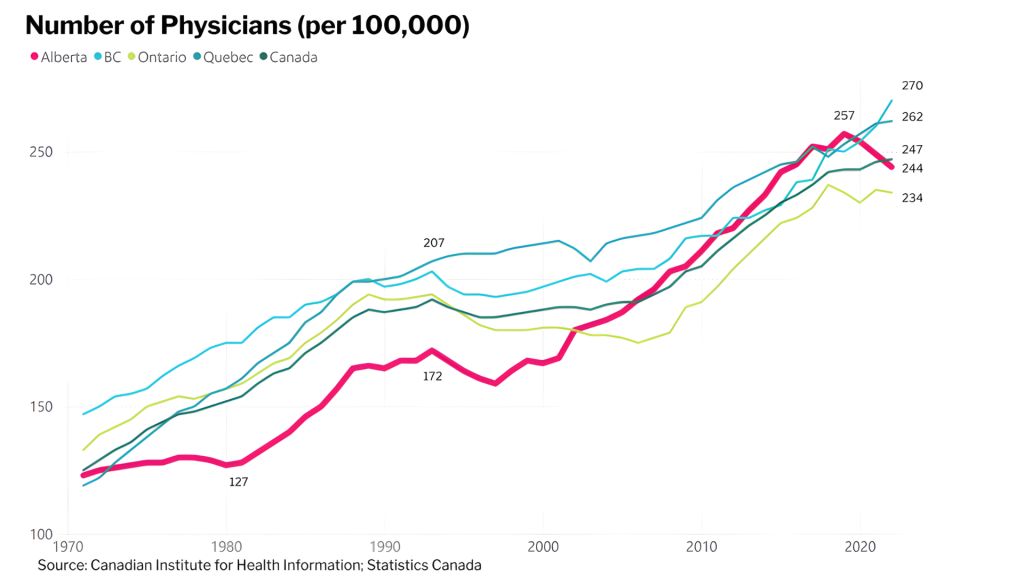
Canada (and Alberta) has far more doctors than in the past. Nationwide, the number of family doctors (GPs) and specialists per capita has doubled since 1971, with Alberta’s growth coming in slightly below that figure. Since 2000, Alberta has seen a 46% increase in the number of resident physicians (as a share of the total population), often having more doctors per capita than BC, Ontario, and the national average from 2013-2020.
How does Alberta compare to other provinces?
On average across Canada, there are 247 doctors per 100,000 residents, while in Alberta, that figure comes in slightly lower, at 244. British Columbia and Nova Scotia have the most doctors per 100,000, at 270 each. By physician type, Alberta is slightly above the national average for specialist physicians and slightly below average for family doctors.
Is there a relationship between wait times and the number of doctors in a province ?
When we talk about wait times, it’s important to mention that there are a few different types of wait times, with each occurring at different stages of a patient’s journey. First, there’s the wait time just to see a family doctor. Then, there’s the time it takes to see a specialist after the family doctor gives a referral. Finally, there’s the time in between seeing the specialist and getting the treatment needed (such as surgery).
Here, we’re just going to focus on the wait time between GP referral and specialist appointment . This is the type of wait time that has seen the largest increase across the country. To be sure, every one of the wait time categories listed above have worsened in the past few decades, but we will only focus on the GP-to-specialist wait time here.
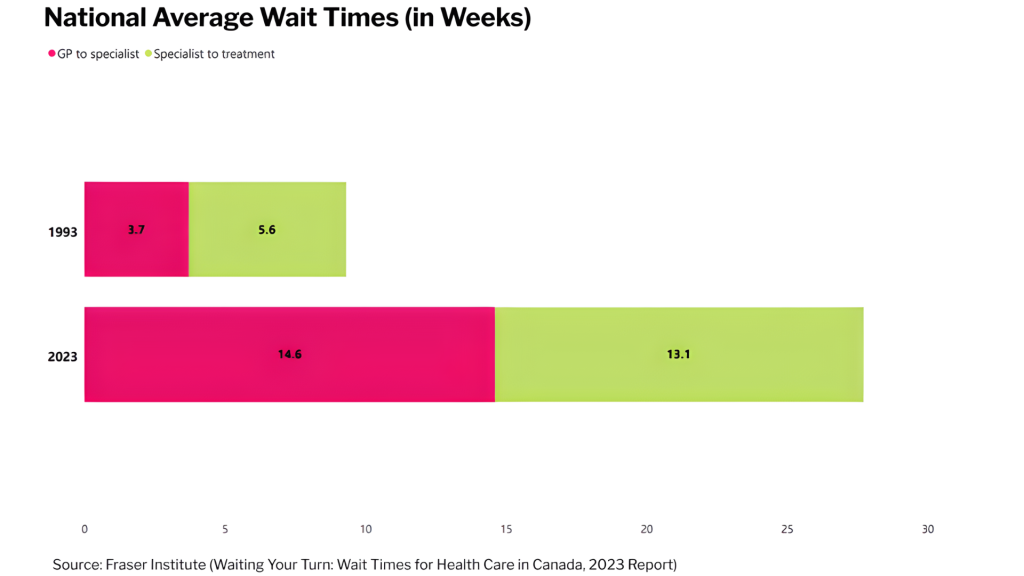
Interestingly, there isn’t a clear relationship between these wait times and the number of doctors working in a province. The number of physicians per capita across Canada has risen by 29% since 1993 but wait times to see a specialist are now almost 4 times longer than they were at the time. In every province, it now takes longer just to get an appointment with a specialist than it did to get treatment from one in 1993.
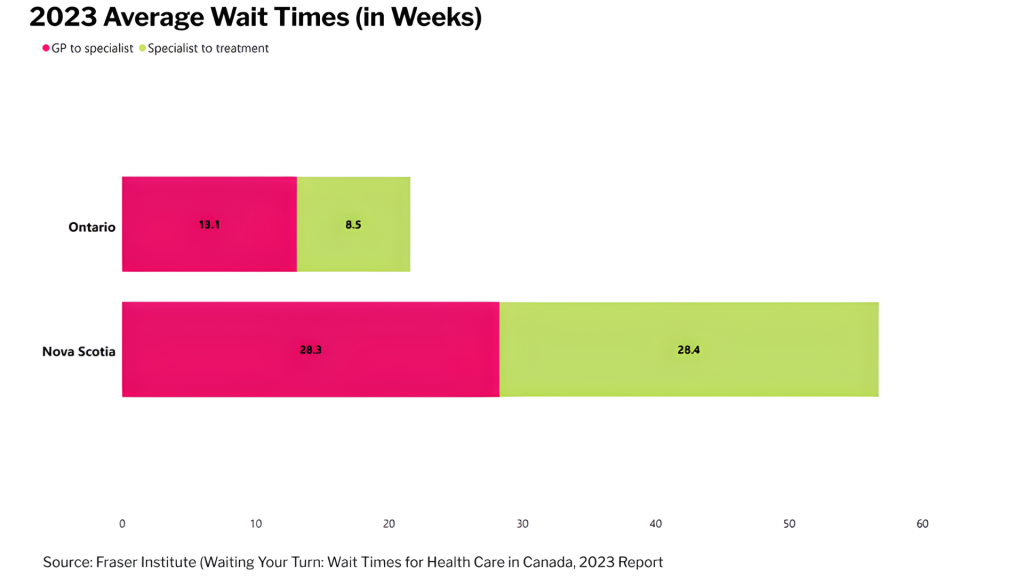
Looking at specific provinces, Nova Scotia has the largest number of doctors per capita, but also the longest wait times in the country. Meanwhile, Ontario ranks poorly in terms of how many doctors per capita compared to other provinces but has the second-shortest GP-to-specialist wait times (and the shortest overall wait times). In fact, it’s faster to get treatment from a specialist in Ontario than it is just to get an appointment with one in Nova Scotia.
Have doctors changed?
One factor behind the increase in wait times is that doctors are working fewer hours than they used to. Between 1988 and 2019, the average number of weekly hours worked by doctors dropped from 53 to 46.
In part, this decline is because there are more female physicians than ever before, and female doctors tend to work fewer hours than their male counterparts. That said, male doctors are working less than before. Female physicians work about 43 hours per week—basically unchanged compared to 30 years ago. Meanwhile, male physicians have reduced their weekly hours from 55 to 47 over that timeframe. Work-life balance, as well as burnout (more on this later) are primary factors behind the decrease.
That said, while doctors may be working fewer hours, the fact remains that there are far more of them than there used to be. In 1988, 185 doctors per capita working 53 hours a week would total 9,805 weekly hours. However, in 2019, 243 doctors per capita working 46 hours a week would total 11,178 weekly hours. Physician hours across Canada have fallen by 13%, but the number of practicing doctors per capita has risen by 31% (and by 56% in Alberta) from 1988 to 2019. In theory, the increase in physician numbers should more than make up for the decline in their working hours.
Have patients changed?
Another factor impacting wait times is demand on the health care system.
More specifically, Canadians (and Albertans) are getting older. And generally speaking, individuals’ use of health care services tends to significantly increase after they reach 65 years of age. 50 years ago, only eight per cent of Canada’s population was over the age of 65. In 2022, that figure was 19 per cent and is expected to increase even further.
While an aging population is certainly a contributing factor, it doesn’t explain everything. The proportion of Canadians over 65 has more than doubled over the last 50 years but there are also more than twice as many doctors per capita, and wait times are almost four times longer. Moreover, countries like Germany, France and Japan have both older populations as well as shorter wait times.
Now we’ll pivot to exploring this issue internationally, and the potential solutions.
How does Canada compare to other countries?
Canada has among the fewest doctors per capita of any OECD country with a universal healthcare system, ahead only of South Korea and Japan. Interestingly, however, those two countries do not have the same issues with wait times as Canada does. And patient satisfaction is significantly higher.
For example, Japan has the fewest doctors per capita of all OECD countries. It also has the largest share of older people in the world—over 50% larger than Canada’s. Even so, it ranks 4th best in terms of the number of doctor consultations per capita—almost twice as many as Canada. Japan also spends less on healthcare than Canada, both on a per capita basis, and as a share of GDP (age-adjusted).
For its part, South Korea has the highest number of doctor consultations per capita, over three times more than Canada, despite having fewer doctors. South Korea also has higher levels of satisfaction on wait times and the quality of their healthcare. Two thirds of Canadians thought that waiting times to get an appointment were too long, while only 39% of Koreans thought the same (the lowest of any country). Finally, 26% of Koreans and only 14% of those in Japan (the lowest of any country) thought their health care system was overstretched, compared to 69% of Canadians.

All this to say, the examples of South Korea and Japan demonstrate that there is not necessarily a direct relationship between the number of physicians in a country on the one hand, and wait times, consultations, and general satisfaction with the health care system on the other.
What can be done to address wait times in Canada?
If adding more doctors isn’t necessarily the answer to solving wait times, what is?
One possibility is to focus on improving the efficiency of health care delivery through options like implementing centralized waiting lists and streamlining administrative processes.
Implementing centralized waiting lists
Something likely to surprise many Canadians is that there is no centralized waiting list or organized system for patient referrals—each doctor and surgeon essentially acts as their own private business and has their own wait list. This means when a doctor refers a patient to a specialist, they’re not consulting a database showing them where the patient can get the quickest care. The referring doctor “usually has no idea whether that specialist has a short or long waiting list.” Instead, referrals are often made by doctors on a “who you know” basis from their personal and professional network.
Under a centralized wait list (sometimes called a “single-entry model”), patients would be automatically matched with the next available specialist. The system is typically optional, meaning that patients could choose to wait for a specific physician if they desired. The Ontario Medical Association says this change alone could reduce wait times by 20 to 30 per cent.
Some provinces are already implementing pilot programs in this area. Alberta’s FAST Program and BC’s Pathways are optional tools available to assist physicians with referrals. And they’re getting results. One study evaluating small versions of these kinds of programs found they result in drastic reductions in wait times, sometimes more than halving them. That said, more comprehensive implementation within (and across) provinces is needed to fully realize the potential gains.
Streamlining administrative processes
Another problem is that doctors across Canada are bogged down in paperwork and bureaucracy. In Nova Scotia, the provincial government found that physicians spend over 500,000 hours on unnecessary administrative tasks per year—the equivalent of 1.7 million patient visits. That’s time that could obviously be better spent reducing backlogs. In Alberta, surveyed doctors said that 40% of their administrative tasks were either unnecessary or could be done by someone else. At the same time, 65% of Alberta doctors have reduced patient slots and half have reduced working hours to cope with the increased administrative burden.
Using the Nova Scotia data mentioned above, the Canadian Federation of Independent Business expanded the study to the rest of Canada, finding that 18.5 million physician hours are spent on unnecessary administrative tasks each year. That’s the equivalent of 55.6 million patient visits. Removing unnecessary paperwork or allowing someone else (or artificial intelligence) to do it for them would allow doctors to make far better use of their time actually referring and treating patients.
Not only is this administrative burden large but it’s also getting worse. Contrary to what someone might think, digitization has not solved the problem (at least not yet); the amount of time physicians spend on administrative tasks per patient has actually increased since the adoption of electronic medical records.
There are many specific problems. One is that medical forms often include redundant and duplicative information entry. Another is that there are significant inefficiencies in the medical records and referrals system. For example, electronic medical records are not integrated or centralized across healthcare providers, with physicians instead having multiple portals for patient information that they struggle to access. On top of that, just over a fifth of doctors are able to exchange clinical patient summaries with physicians outside of their practice.
A high administrative burden is one of the primary factors contributing to doctors working fewer hours, and to physician burnout in general. Burnout, specifically, is a concern affecting the majority of doctors across the country, and has both immediate and downstream effects that impact wait times and the quality and availability of care. In Alberta alone, 4 out of 5 primary care physicians are considering retirement or leaving the profession altogether simply because of the administrative burden.
The bottom line
Solving Canada’s wait times problem is not just a matter of hiring more doctors. While that would almost certainly help, there are other issues affecting wait times that shouldn’t be overlooked. Specifically, focused reforms in specific areas of the health care system would yield significant efficiency gains, allowing doctors to focus on their most important task (caring for patients), supported by systems that make that process as streamlined as possible.


